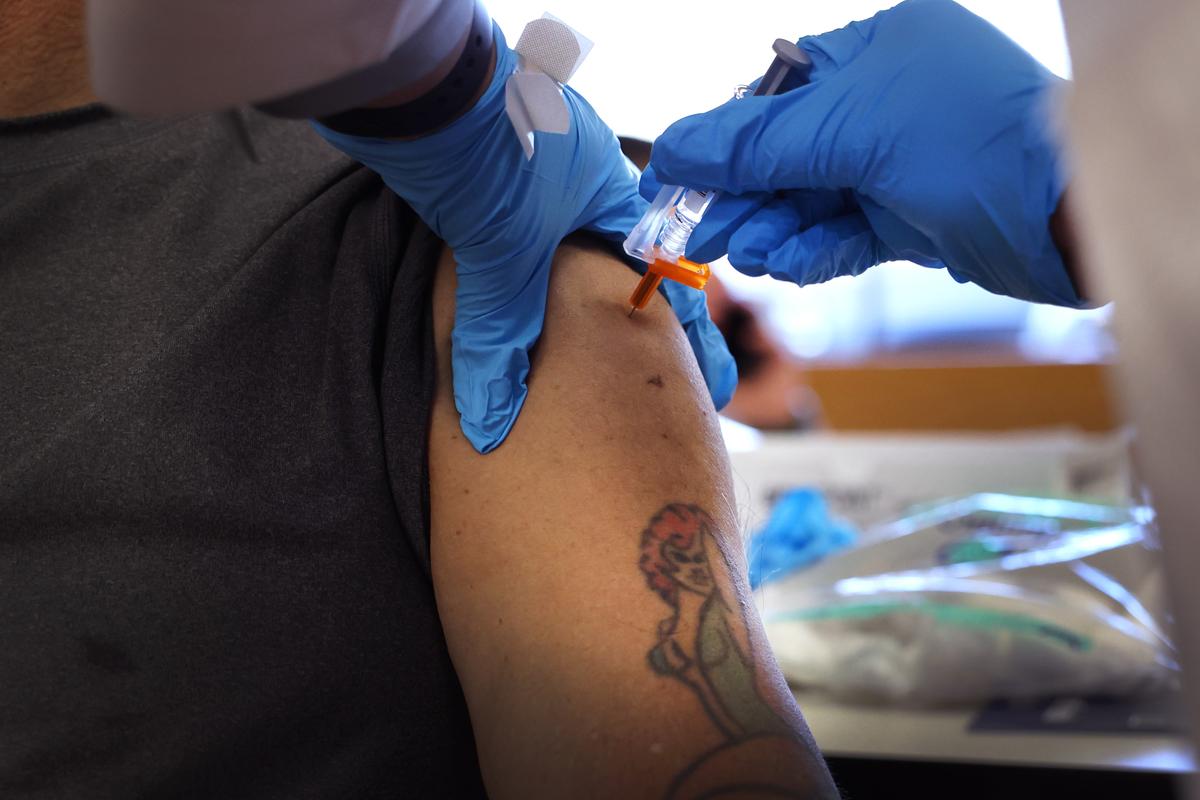
A growing number of studies indicate people are at higher risk of stroke if they receive COVID-19 and influenza vaccines at the same time, though other papers have not found an elevated risk.
The link between the vaccines and stroke, according to authorities, is not yet proven, but some experts say the papers boost the position of spacing out shots to reduce the risk of side effects.
“Oftentimes, we suggest if you want to minimize the chance of interactions and minimize confusing side effects from one with another, you wait about two weeks between the vaccines," he said.
Dr. David Boulware, an infectious disease expert at the University of Minnesota Medical School, told The Epoch Times in an email that he generally recommends receiving the COVID-19 and influenza vaccines on separate occasions "so as to not have one vaccine blunt the response of the other."
Uncertainty
Other papers have found no elevated risk for the COVID-19 vaccines and stroke, including a study in England that examined simultaneous COVID-19 vaccination and influenza vaccination. The COVID-19 vaccines analyzed in the study were versions never administered in the United States."Available data do not provide clear and consistent evidence of a safety problem for ischemic stroke with bivalent mRNA COVID-19 vaccines when given alone or given simultaneously with influenza vaccines, or when influenza vaccine is given alone," Dr. Tom Shimabukuro, a CDC vaccine safety official, told a panel of the agency's advisers on Oct. 25 as he went over the papers from the FDA, Kaiser Permanente, and England.
The researchers that have found an elevated risk say further research is required to validate the signals.
"The potential association between bivalent COVID-19 vaccination and ischemic stroke .... warrants further investigation among individuals," the Kaiser Permanente researchers said in their preprint paper.
The self-controlled case series only examined stroke incidents among vaccinated people. The researchers compared the incidence of stroke in people the first 42 days after vaccination with the incidence in the same people in the time beyond that.
They identified 373 strokes within 42 days of bivalent vaccination and 1,511 after 42 days.
The elevated risk was found among people younger than 65 who received a Pfizer or Moderna vaccine, had a history of COVID-19, and received an influenza vaccine at the same time.
An elevated risk was also found among the same age group in people who received Pfizer's shot with an influenza shot and did not have a history of COVID-19, and people who received Moderna's shot, had a history of COVID-19, and did not receive an influenza vaccine concomitantly.
The FDA researchers also conducted a self-controlled case series among Medicare beneficiaries, excluding unvaccinated people. They used risk intervals within 42 days after vaccination and a control interval of 43 to 90 days after a shot.
The researchers identified elevated risks of non-hemorrhagic stroke and non-hemorrhagic stroke/transient ischemic attack among Pfizer recipients 85 and older, and non-hemorrhagic stroke/transient ischemic attack in Moderna recipients aged 65 to 74.
There was also an increased risk of non-hemorrhagic stroke among all recipients, who are 65 and older, 22 to 42 days after concomitant high-dose/adjuvanted influenza and Pfizer vaccination, and an elevated risk of transient ischemic attack one to 21 days after concomitant high-dose/adjuvanted influenza and Moderna vaccination.
Dr. Boulware, who was not involved in the research, said he'd like to see the findings replicated by other researchers.
The
FDA researchers said that their study did not alter the agency's
position that the benefits of the COVID-19 outweigh their risks in the
elderly, but did indicate a "need for additional investigations" into
the safety of high-dose/adjuvanted influenza vaccines. The Australian
researchers said their study supported coadministering Pfizer's vaccine
with an influenza vaccine.





No comments:
Post a Comment