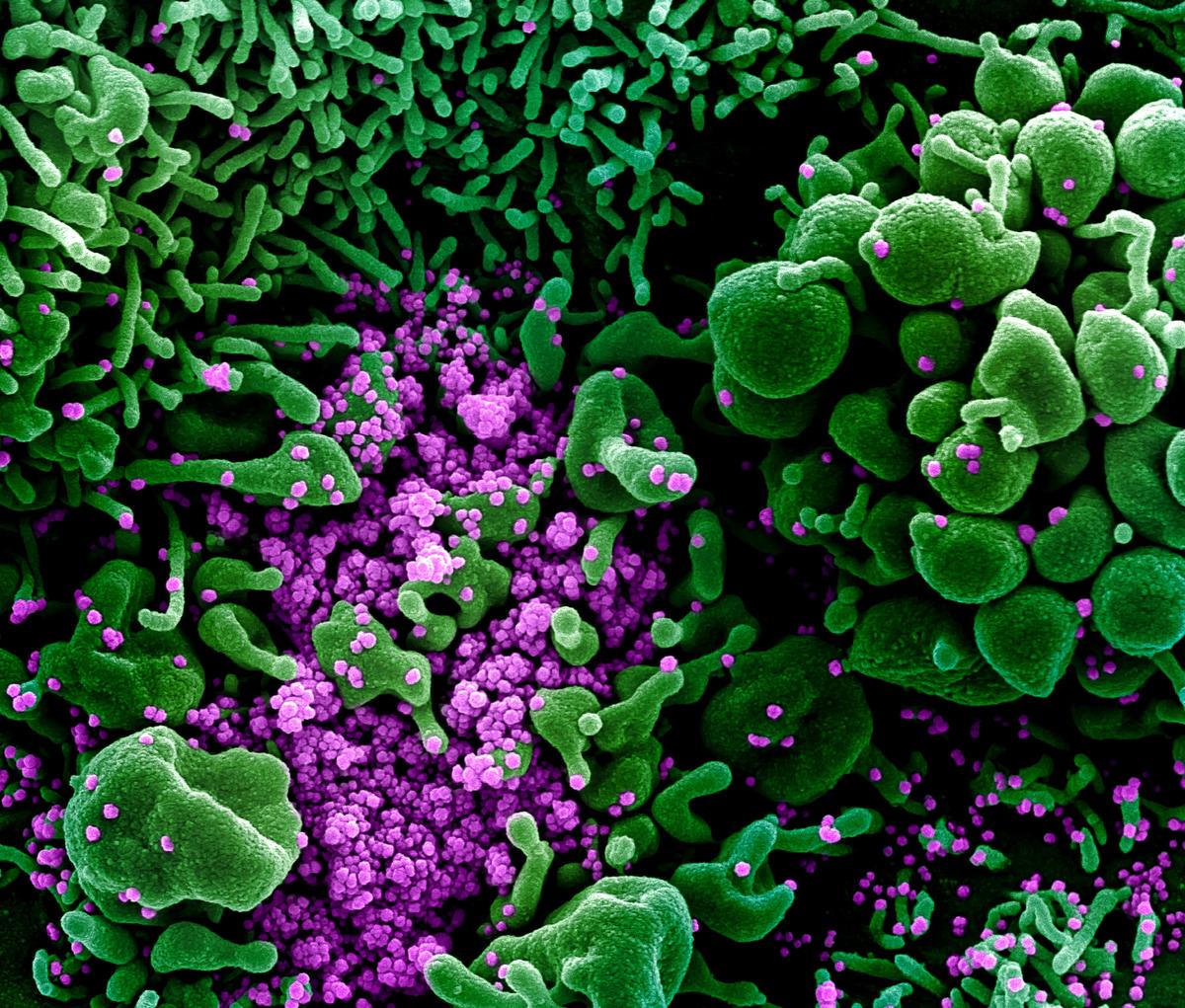
Colorized scanning electron micrograph of cell (green) heavily infected
with COVID-19 particles (purple), commonly known as SARS-CoV-2 or novel
CCP virus, isolated from a patient sample on March 16, 2020. (NIAID)
COVID-19 vaccines can trigger genetic changes in cancer patients that could aid in the further development of the disease in such individuals, according to a recent peer-reviewed analysis.
The conclusion was based on two factors. First is the “multi-hit hypothesis” of cancer, which suggests that cancer is the consequence of several genetic mutations.
The second is the “growing evidence and safety reports” in the Vaccine Adverse Effects Report System (VAERS), which suggested that some cancer patients who took COVID-19 vaccines saw their conditions worsen.
“In light of the above and because some of these concerns also apply to cancer patients infected with SARS-CoV-2, we encourage the scientific and medical community to urgently evaluate the impact of both COVID-19 and COVID-19 vaccination on cancer biology and tumor registries, adjusting public health recommendations accordingly,” the review said.
The review focused on mRNA vaccines, Pfizer/BioNTech and Moderna, and adenovirus-vectorized vaccines, Johnson & Johnson and Oxford/AstraZeneca, as these products were most widely used in global COVID-19 vaccination campaigns.
mRNA vaccines have the potential to trigger a set of biological mechanisms that could lead to the progression of cancer, it said.
These effects are attributed to factors like the “pro-inflammatory action” of lipid nanoparticles (LNPs) and tumor-causing effects of the vaccines’ antigens, namely the spike protein.
LNPs are nanoparticle drug delivery systems that can be used to deliver DNA and mRNA into a body. The spike protein, found on the surface of the COVID-19 virus, facilitates the entry of the virus into healthy cells.
The authors who wrote the review are Raquel Valdes Angues from the Oregon Health and Science University School of Medicine in Portland and Yolanda Perea Bustos from the education department in the Government of Catalonia, Barcelona, Spain. They declared “no financial support” from organizations that might have an interest in their work and no other relationships or activities that could have influenced the review.
The analysis outlined several genetic effects that COVID-19 vaccines could have on cancer cells and thereby potentially negatively impact the lives of patients suffering from the illness.
Lymphopenia
The review noted that COVID-19 vaccination has been associated with lymphopenia—a condition in which there is an abnormally low count of lymphocytes, a type of white blood cell that helps the immune system fight against foreign bacteria and viruses.Clinical trials of the Pfizer and AstraZeneca vaccine described a “decrease in plasma lymphocytes 6-8 days post-vaccination in 45 percent-46 percent of participants.”
“Lymphopenia has long been associated with increased cancer incidence and risk of malignancy,” said the review. “Lymphocyte alterations are frequent in patients with cancer and strongly impact prognosis and survival.”
Spike Proteins
The spike protein present in COVID-19 coronaviruses has two key functional subunits—S1 and S2. S1 helps the virus in infecting human cells and has been found to affect the mechanism of cell growth.Meanwhile, the spike protein has been shown to influence a mechanism that regulates several key cellular behaviors, specifically inflammatory responses and cellular growth. When activated in cancer cells, this specific mechanism promotes chemoresistance and proliferation. In a tumor microenvironment, it stimulates immune suppression.
Compromising Immunity
Researchers suggested that mRNA vaccines are “designed to deactivate” an individual’s innate immunity.The innate immune system of mammals is stimulated through the activation of a class of proteins called Toll-like receptors (TLRs). TLRs are known to trigger several signaling pathways for the production of various cytokines that play an important role in many diseases, including cancer.
The signaling pathways involve IFN regulatory factors (IRFs) critical in several aspects of immune response. The review cited research showing that Pfizer COVID-19 vaccines “significantly decreased” the production of type I IFN and type II IFN.
TLRs are not only expressed in immune cells but also in tumor cells, in which they can either promote or inhibit malignancy. Type I IFN has also been found to be important in controlling the growth of tumors and in the response to anti-tumor therapies.
Inflammatory
The lipid nanoparticles (LNP) used in the mRNA vaccines have been found to be “highly inflammatory” in mice, the review said, citing a report.In the context of cancer, inflammation is conducive to the development of the disease and promotes all stages of tumorigenesis—the initial formation of a tumor in an individual.
“Around 15 percent-20 percent of all cancer cases are preceded by infection, chronic inflammation, or autoimmunity at the same tissue or organ site,” the review stated. “In such cases, cancer-promoting inflammation is induced and exists long before tumor formation.”
Such extrinsic inflammation—referring to inflammation caused by outside sources—can result in immunosuppression, where the immune system becomes temporarily dysfunctional. This immunosuppression can provide the environment for the development of tumors.
Genomic Integration
The review highlighted a study discussing the possibility that certain parts of the COVID-19 virus might undergo “genomic integration within infected cells.”The study found copies of the virus in human cells and speculated that the same phenomenon could occur once human cells are exposed to COVID-19 mRNA vaccines.

The review speculated that the mRNA vaccine’s impact on LINE-1 might “enhance the risk of mutations in tumor suppressor genes and lead to sustained DNA damage in cells and tissues targeted by the vaccine.”
Tumor Suppression
An October 2020 study showed that the S2 subunit of the COVID-19 virus “strongly interacts” with tumor suppressor proteins p53 and BRCA1/2, said the review.Proteins like p53 and BRCA1/2 act as a “major barrier” to tumor progression. The possibility that the virus’ spike protein can interact with tumor suppressor protein is critical since both mRNA and adenovirus-vectorized vaccine contain the “genetic material that instructs the host cells to express spike.”
Studies on the Pfizer vaccine have shown that it accumulates in various organs within 48 hours of vaccination. In addition, lipid nanoparticles “preferentially accumulate” in the tumor tissue rather than the healthy tissue.
Given these findings, the review suggested a detailed look into the potential interactions between S2 and tumor suppressor proteins p53 and BRCA1/2 in both COVID-19 patients and those who have received COVID-19 vaccination.
Such an analysis is necessary to determine if the interactions provide a “selective advantage” for cancer or precancerous cells, the researchers wrote.
‘Dubious’ Vaccination Benefits
The researchers noted that they have shown COVID-19 spike protein-based vaccines to “have the potential to interact with tumor suppressor proteins, promote inflammation, activate oncogenic pathways, and disrupt the fine-tuning of the immune response.”“These dysregulated mechanisms and signaling pathways underlie most types of cancer.” A more “balanced risk/benefit evaluation is urgently needed” regarding COVID-19 vaccination and people with or at high risk of cancer.
For people with poor immune responses, “the benefits of vaccination are dubious, and the cumulative risks of successive boosters are unknown.”

An area of concern is that the co-administration of anticancer treatments and COVID-19 vaccines could pave the way for “toxic effects.” The review cited an article that found that when cancer patients were given Pfizer’s COVID-19 vaccine, there was a “constant and variable increase of all COVID-19 vaccination side effects.”
“There is thus a concern that the simultaneous use of immunotherapy and COVID-19 vaccines boosts the body’s immune response, resulting in enhanced immune-related adverse events,” the researchers wrote.
The review stated that between Jan. 7, 2018, and July 2, 2022, there were approximately 13,000 cancer deaths per week in the United States, with peaks occurring in January 2021 and January 2022. While public health agencies have admitted a rise in cancer deaths, they have mostly attributed the excess deaths to the COVID-19 infection.
Even though cancer mortality peaks in 2021 and 2022 correlate with COVID-19 winter surges, “they also follow two major COVID-19 vaccination and booster campaigns,” the researchers pointed out.
“As noted earlier, both SARS-CoV-2 and SARS-CoV-2 spike protein-based vaccines promote the production of spike within human cells, which, in light of the above, might facilitate malignant transformation.”
The authors noted that even though many institutions and experts promote COVID-19 vaccines as safe and effective in patients with cancer, “these claims are unsupported.”
“Our suggestion is that individuals with cancer or a history of cancer should receive the genetic COVID-19 vaccines only if the benefits clearly outweigh any risks and after careful evaluation case by case,” said the review.
“Most importantly, there is the possibility that cancer risk is dose-dependent.” As such, only individuals who have taken multiple COVID-19 immunizations may be at higher risk of cancer malignancy.
“The success of the novel mRNA-based vaccines against COVID-19 has created a widespread interest in mRNA technology as a solution to some of the deadliest infectious diseases (i.e., malaria, tuberculosis, and HIV/AIDS) for which an effective and easily deployable vaccine is urgently needed,” the authors wrote.
However, “current
safety concerns should be promptly addressed before mRNA-based
nanomedicines further transform the way diseases are managed and
prevented in the future.



No comments:
Post a Comment